Bladder Irrigation Procedure: A Comprehensive Guide
Bladder irrigation, a vital nursing skill, demands meticulous attention to detail for optimal patient outcomes, encompassing both continuous and intermittent techniques.
Bladder irrigation is a crucial procedure employed in healthcare settings to maintain urinary tract patency and address various clinical scenarios. It involves instilling fluid into the bladder and subsequently draining it, effectively cleansing the bladder and urethra. This technique is particularly valuable post-operatively, in cases of hematuria, or when urinary retention occurs.
Effective bladder irrigation requires a thorough understanding of the procedure, diligent monitoring for potential complications like fluid overload or infection, and adherence to established best practices. Nurses play a pivotal role in ensuring safe and successful irrigation, consistently documenting observations and patient responses. Maintaining drainage system integrity and consistent catheter care are paramount to minimizing risks and promoting patient comfort.
What is Bladder Irrigation?
Bladder irrigation is a process of introducing sterile fluid into the bladder through an indwelling urinary catheter, followed by its drainage. This flushing action aims to clear the bladder and urethra of blood clots, sediment, or mucus, restoring optimal urinary flow. It’s a therapeutic intervention, not a cure, addressing symptoms and preventing complications.
The procedure can be performed continuously, using a three-way catheter, or intermittently, with manual instillation and drainage. Careful monitoring of urine output, color, and the presence of clots is essential. Proper technique minimizes the risk of trauma and infection, ensuring patient safety and comfort throughout the process. Consistent documentation of all aspects of the irrigation is vital for comprehensive patient care.
Types of Bladder Irrigation
Bladder irrigation presents in two primary forms: Continuous Bladder Irrigation (CBI) and Intermittent/Manual Bladder Irrigation. CBI utilizes a three-way catheter, maintaining a constant flow of sterile solution into and out of the bladder. This is ideal for managing persistent clots or bleeding post-operatively.
Conversely, intermittent irrigation involves manually instilling and draining fluid as needed, often after surgery or to address temporary obstruction. The choice depends on the clinical situation and patient needs. Both methods require strict aseptic technique to prevent infection. Regular catheter care and meticulous documentation are crucial components of either approach, ensuring optimal patient outcomes and minimizing potential complications.
Continuous Bladder Irrigation (CBI)
Continuous Bladder Irrigation (CBI) employs a three-way Foley catheter, maintaining constant fluid flow. Sterile irrigation solution prevents clot formation and ensures continuous bladder drainage. Nurses meticulously record urine output with each flask change, documenting color, clarity, and the presence of clots.
Regular catheter care is paramount, minimizing the risk of Catheter-Associated Urinary Tract Infections (CAUTI). Maintaining the drainage bag below bladder level and preventing tubing obstructions are essential. Accurate documentation in progress notes and care plans, including patient comfort levels and irrigation fluid tolerance, is vital for comprehensive patient management and effective monitoring during CBI.
Intermittent/Manual Bladder Irrigation
Intermittent or manual bladder irrigation involves instilling sterile solution into the bladder via a catheter, followed by drainage. This technique is utilized to clear clots or medicate the bladder. Nurses must ensure a clear understanding of the procedure’s rationale and thoroughly educate patients about its purpose and process.
Proper documentation is crucial, detailing the volume of irrigant used, the characteristics of the returned fluid (color, clarity, presence of clots), and any patient discomfort experienced; Consistent adherence to CAUTI prevention protocols, alongside appropriate order verification, guarantees safe and effective implementation of this valuable technique.
Indications for Bladder Irrigation
Bladder irrigation addresses post-operative care, hematuria management, urinary retention, and clot prevention, ensuring optimal urinary tract function and patient recovery.
Post-Operative Care
Following surgeries involving the bladder or lower urinary tract, irrigation plays a crucial role in maintaining patency and removing blood clots. Post-operative bladder irrigation helps prevent obstruction of the urinary catheter, ensuring continuous drainage and minimizing the risk of bladder distension.
This is particularly important after procedures like Transurethral Resection of the Prostate (TURP) or bladder tumor resection, where bleeding and clot formation are common. Consistent irrigation facilitates clear urine output, allowing for accurate assessment of kidney function and overall fluid balance.
Nurses must diligently monitor urine characteristics, noting color, clarity, and the presence of any clots, documenting findings meticulously in the patient’s chart. Proper post-operative irrigation contributes significantly to a smoother recovery and reduces the likelihood of complications.
Hematuria Management
Bladder irrigation is a cornerstone in managing hematuria, particularly when significant bleeding occurs, preventing clot formation that could obstruct urinary flow. Continuous bladder irrigation (CBI) is frequently employed to flush out blood and debris, maintaining a clear urinary passage and reducing patient discomfort.
Effective hematuria management necessitates careful monitoring of urine output, assessing the degree of hematuria, and ensuring adequate hydration to dilute the urine. Nurses play a vital role in titrating the irrigation rate to achieve optimal clearance without causing bladder spasms or excessive fluid shifts.
Prompt intervention with irrigation can minimize the need for more invasive procedures and support the resolution of bleeding episodes, improving patient well-being.
Urinary Retention
Bladder irrigation serves as a crucial intervention for urinary retention, especially post-operatively or when obstructions hinder natural bladder emptying. Intermittent or manual bladder irrigation can effectively evacuate retained urine, alleviating bladder distension and associated discomfort.
The procedure involves carefully instilling sterile irrigation solution into the bladder, followed by gentle drainage, ensuring complete evacuation without forceful manipulation. Nurses must assess the patient’s bladder volume and monitor for signs of discomfort or bladder spasms during the process.
Successful irrigation restores normal bladder function, prevents complications like urinary tract infections, and promotes patient comfort and recovery.
Prevention of Clot Formation
Bladder irrigation plays a pivotal role in preventing clot formation, particularly following surgeries involving the bladder or prostate, or in patients experiencing hematuria. Continuous bladder irrigation (CBI) maintains consistent fluid flow, effectively flushing out blood clots before they can organize and obstruct the urinary catheter or bladder neck.
Maintaining adequate irrigation flow rates, as determined by the height of the infusion set, is crucial for clot removal. Nurses must diligently monitor urine output for clot presence and document any instances requiring manual bladder washout.
Proactive clot prevention minimizes the risk of catheter blockage and subsequent urinary retention, promoting optimal patient recovery.
Procedure Preparation
Thorough preparation includes verifying physician orders, gathering necessary equipment, assessing the patient, and providing clear education about the procedure.
Equipment Checklist
Essential equipment for bladder irrigation includes a sterile irrigation solution (typically normal saline), an irrigation tray with sterile gloves, catheter insertion tray if needed, and a graduated cylinder for accurate fluid measurement. A sterile catheter, appropriate size, is crucial, alongside drainage bags – one for urine and one for irrigation fluid – ensuring they are positioned correctly.
Additional supplies encompass sterile drapes, antiseptic solution for catheter site care, tape, and measuring containers to monitor input and output. Importantly, have a syringe available for manual irrigation if indicated. Documentation tools, including flow sheets and patient charts, are also vital. Finally, ensure availability of appropriate personal protective equipment (PPE) for healthcare personnel.

Patient Assessment & Education
Prior to irrigation, a thorough patient assessment is paramount, including vital signs, urinary output, pain levels, and a review of medical history, particularly focusing on allergies and bleeding disorders. Assess the patient’s understanding of the procedure and address any anxieties.
Patient education should explain the purpose of the irrigation, what to expect during and after the procedure, and the importance of reporting any discomfort or unusual symptoms. Emphasize the need for adequate hydration and the rationale behind maintaining proper catheter care; Clearly communicate the potential risks and benefits, fostering informed consent and collaboration.
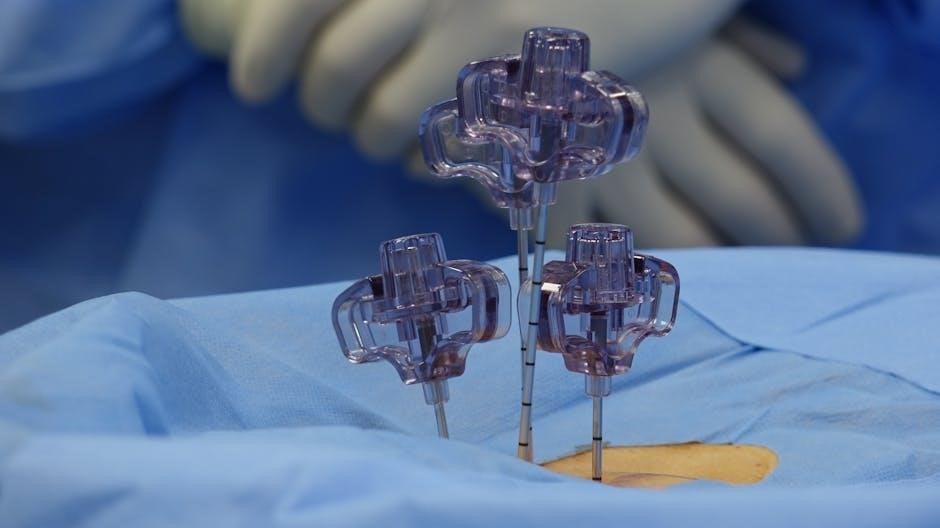
Order Verification
Before initiating bladder irrigation, meticulous verification of the physician’s order is crucial. Confirm the type of irrigation prescribed – continuous or intermittent – along with the specific irrigation solution, rate, and duration. Validate any associated parameters, such as desired urine output or clarity goals.
Ensure the order aligns with the patient’s clinical condition and documented indications. Double-check for contraindications, such as bladder perforation or recent bladder surgery. Proper order verification minimizes errors and ensures patient safety, adhering to established protocols and institutional guidelines. Document the verification process in the patient’s chart.
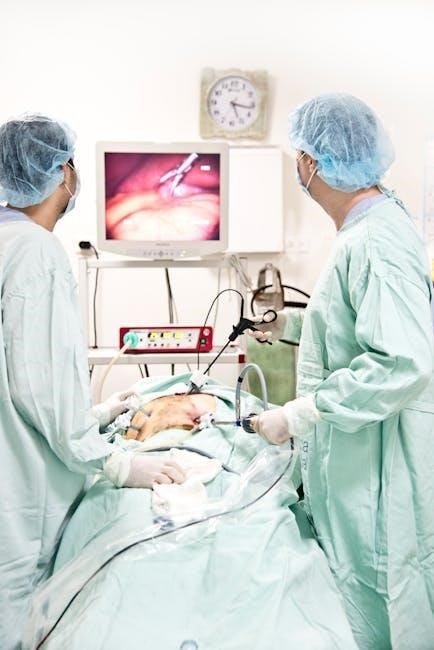
Performing Continuous Bladder Irrigation (CBI)
CBI involves maintaining a constant flow of irrigation solution through the bladder, meticulously balancing inflow and outflow to clear clots and debris.
Setting Up the Irrigation Solution
Preparing the irrigation solution is a critical first step. Typically, sterile normal saline is utilized, warmed to body temperature to minimize bladder spasms and patient discomfort. The solution volume is determined by the physician’s order, often ranging from 500ml to 1 liter per irrigation cycle.
Ensure the IV tubing is dedicated solely for irrigation purposes, preventing contamination. Prime the tubing meticulously, eliminating all air bubbles to avoid introducing air into the bladder. Securely connect the tubing to the irrigation solution bag and then to the urinary catheter insertion site, maintaining a closed sterile system.
Confirm the flow rate as prescribed, carefully observing for any leaks or disruptions in the system. Document the solution type, volume, and start time in the patient’s medical record;
Maintaining Fluid Balance
Diligent fluid balance monitoring is paramount during continuous bladder irrigation (CBI) to prevent complications like fluid overload or electrolyte imbalances. Accurate intake and output recording is essential, meticulously documenting both the irrigation fluid infused and the urine output drained.
Assess the patient frequently for signs of fluid overload, including edema, shortness of breath, and elevated blood pressure. Monitor electrolyte levels, particularly sodium, as continuous irrigation can dilute serum concentrations.
Adjust the irrigation flow rate as needed, guided by the patient’s urine output and overall fluid status. Communicate any significant changes or concerns to the physician promptly, ensuring timely intervention and patient safety.
Monitoring Urine Output
Consistent and precise urine output monitoring is crucial during bladder irrigation, especially CBI, to assess the procedure’s effectiveness and identify potential complications. Record the amount of irrigation fluid used and the urine returned with each interval, noting any discrepancies.
Observe urine color and clarity, documenting the degree of hematuria or the presence of clots. A decrease in urine output or a sudden increase in blood content warrants immediate attention and physician notification.
Regularly assess the drainage tubing for kinks or obstructions that could impede urine flow. Accurate documentation of urine characteristics and volume is vital for evaluating treatment progress and guiding further interventions.
Catheter Care During CBI
Diligent catheter care is paramount during continuous bladder irrigation to minimize the risk of catheter-associated urinary tract infections (CAUTI). Perform regular perineal hygiene, ensuring the insertion site is clean and dry. Secure the catheter to prevent movement and trauma to the urethra.
Maintain the drainage bag below bladder level to promote gravity drainage and prevent backflow. Prevent any obstructions or dependent loops in the tubing, ensuring continuous irrigation.
Document all catheter care provided, including patient comfort levels, urine color, degree of hematuria, and any observed clots. Consistent adherence to CAUTI prevention protocols is essential.
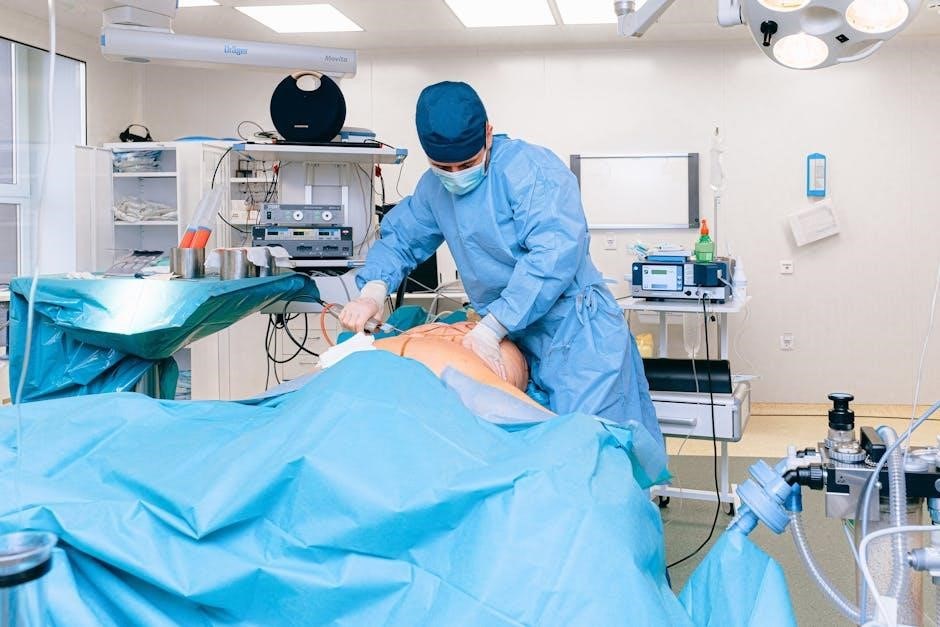
Performing Intermittent/Manual Bladder Irrigation
Manual bladder irrigation involves instilling and draining fluid, requiring careful technique and assessment of urine output for clot presence and clarity.
Instillation Technique
Prior to instillation, verify the healthcare provider’s order and gather necessary supplies. Position the patient comfortably, typically supine, and maintain strict aseptic technique throughout the procedure. Gently insert a lubricated catheter into the bladder, ensuring proper placement.
Slowly instill the prescribed irrigation solution – often normal saline – using gentle pressure. Avoid forceful injection to prevent bladder trauma. The amount instilled depends on the clinical situation and physician orders. After instillation, briefly clamp the catheter to allow the solution to dwell, loosening any sediment or clots.
Observe for any patient discomfort during instillation, and immediately discontinue if pain occurs. Proper technique minimizes risk and maximizes effectiveness of the irrigation process.
Drainage and Assessment
Following instillation, unclamp the catheter and allow for complete drainage of both the instilled fluid and the patient’s urine. Carefully observe the characteristics of the returned fluid, noting the color, clarity, and presence of any sediment, blood clots, or particulate matter. Document these findings meticulously in the patient’s chart.
Accurate urine output measurement is crucial, and should be recorded on the fluid balance chart. Assess the patient for any signs of discomfort, bladder spasms, or leakage around the catheter. Report any abnormalities to the healthcare provider promptly.
Regular assessment ensures effective irrigation and early detection of potential complications, contributing to optimal patient care and recovery.
Documentation of Procedure
Comprehensive documentation is paramount for continuity of care and legal protection. Record the date, time, and type of bladder irrigation performed (continuous or intermittent) in the patient’s medical record. Detail the volume of irrigation solution used, the amount and characteristics of urine returned – including color, clarity, and presence of clots.
Document patient tolerance of the procedure, noting any discomfort, bladder spasms, or leakage. Include any interventions performed, such as repositioning or administering pain medication.
Record catheter care provided, including the date and time, and any observations made regarding the catheter site. Accurate and thorough documentation ensures clear communication among healthcare team members.

Potential Complications & Monitoring
Vigilant monitoring is crucial to detect fluid overload, electrolyte imbalances, CAUTI, and bladder trauma, requiring prompt intervention and careful assessment.
Fluid Overload
Fluid overload represents a significant risk during continuous bladder irrigation (CBI), stemming from the continuous infusion of irrigation solution. Nurses must meticulously monitor patients for signs and symptoms, including edema, shortness of breath, elevated blood pressure, and crackles in the lungs.
Accurate intake and output documentation is paramount, alongside frequent assessment of the patient’s cardiovascular and respiratory status. Adjusting the irrigation flow rate, as prescribed, is essential to balance fluid input and output. Promptly reporting any concerning changes to the physician ensures timely intervention, potentially involving diuretic administration or fluid restriction to mitigate the risk of pulmonary edema and other complications associated with fluid excess.
Electrolyte Imbalance
Electrolyte imbalances can occur during prolonged bladder irrigation, particularly with continuous methods, due to the absorption of irrigation fluid. Frequent monitoring of serum electrolyte levels – including sodium, potassium, and chloride – is crucial. Hypo- or hypernatremia can manifest with neurological changes, muscle weakness, or cardiac arrhythmias.
Nurses should be vigilant for signs of electrolyte disturbances and collaborate with the healthcare team to implement corrective measures, such as electrolyte replacement therapy. Utilizing an irrigation solution with appropriate electrolyte concentrations, as prescribed, helps minimize the risk. Careful assessment of the patient’s renal function is also vital, as impaired kidney function exacerbates the potential for electrolyte imbalances during bladder irrigation.
Catheter-Associated Urinary Tract Infections (CAUTI)
Catheter-associated urinary tract infections (CAUTI) represent a significant risk during bladder irrigation, especially with continuous irrigation. Maintaining strict aseptic technique during catheter insertion and irrigation fluid changes is paramount. Regular catheter care, including perineal hygiene, minimizes bacterial colonization.
Implementing a CAUTI prevention bundle – keeping the drainage bag below bladder level, preventing tubing obstructions, and daily catheter care – is essential. Nurses must diligently document catheter care provided, noting urine characteristics and patient comfort. Prompt recognition and reporting of signs of infection, such as fever, dysuria, or cloudy urine, are crucial for timely intervention and antibiotic administration.
Bladder Trauma & Infection Transmission
Bladder trauma, though infrequent, is a potential complication of bladder irrigation, particularly with forceful instillation or pre-existing bladder pathology. Careful technique and appropriate irrigation solution pressure are vital to prevent mucosal damage. Vigilant monitoring for hematuria or signs of bladder perforation is necessary.
Infection transmission poses a risk if aseptic technique is compromised. Healthcare providers must adhere to strict hand hygiene protocols and utilize sterile equipment for all aspects of the procedure. Proper handling and disposal of contaminated materials are crucial. Maintaining a closed irrigation system minimizes bacterial entry, safeguarding patient safety and preventing healthcare-associated infections.
Nursing Considerations & Best Practices
Prioritize consistent CAUTI prevention, maintain drainage integrity, document meticulously, and consider CBI flow rates to optimize patient safety and outcomes.
CAUTI Prevention Bundle
Implementing a robust CAUTI prevention bundle is paramount when managing bladder irrigation, particularly Continuous Bladder Irrigation (CBI). This multifaceted approach centers on minimizing the risk of catheter-associated urinary tract infections. Key components include consistently maintaining the drainage bag below the level of the patient’s bladder to prevent backflow and bacterial migration.
Furthermore, diligent attention must be paid to preventing any obstructions or dependent loops within the tubing, ensuring unimpeded urine flow. Regular, scheduled catheter care, performed daily, is also crucial. Thorough documentation within the patient’s progress notes and care plan is essential, detailing observations such as patient comfort levels, urine color, the degree of hematuria, urine output volumes, and the presence of any clots requiring manual bladder washout.
Maintaining Drainage System Integrity
Ensuring the continuous functionality of the bladder irrigation drainage system is critical for effective therapy and preventing complications. Regularly assess the tubing for kinks, knots, or obstructions that could impede urine flow and increase the risk of bladder distension or reflux. The drainage bag should remain positioned below bladder level at all times, preventing backflow and potential infection.
Consistent monitoring of the system is vital; promptly address any leaks or disruptions. Proper securement of the catheter and tubing minimizes accidental dislodgement. Document any interventions or issues related to the drainage system in the patient’s chart. A functioning, intact system directly contributes to accurate urine output measurement and reduces the likelihood of catheter-associated complications.
Regular Catheter Care Documentation
Thorough and consistent documentation of catheter care is paramount for comprehensive patient management during bladder irrigation. Record details of each care event, including the date, time, and specific interventions performed, such as cleaning of the meatus and catheter securement. Meticulously document urine characteristics – color, clarity, and the presence of clots or sediment – alongside accurate urine output measurements.
Note any patient discomfort or signs of irritation at the insertion site. Document if manual bladder washout was necessary and the results obtained. Comprehensive records facilitate effective communication among healthcare team members and provide a clear audit trail for quality assurance and potential complication tracking.
Flow Rate Considerations for CBI
Maintaining an appropriate flow rate is crucial during Continuous Bladder Irrigation (CBI) to effectively remove clots and prevent bladder thrombosis. Nurses must carefully assess and adjust the irrigation infusion set height, understanding its direct impact on fluid dynamics. Continuous monitoring ensures adequate drainage of irrigation fluid, preventing backflow and maintaining bladder patency.
The flow rate should be sufficient to clear debris without causing excessive bladder distension or trauma. Regular assessment of urine output and irrigation fluid balance is essential to prevent complications like fluid overload. Careful consideration of these factors optimizes CBI effectiveness and minimizes potential risks for the patient.